
Benign rolandic epilepsy is actually an idiopathic epileptic syndrome that causes nocturnal seizures with focal onset and diurnal partial seizures stemming from the lower rolandic area which are characterized by a specific EEG pattern. In children seizures of this type may occur during the day or at night but are more reported to occur at night. Some patients wake up while others continue sleeping as if nothing has happened. Only parents or people who are near may notice the presence of an epileptic attack.
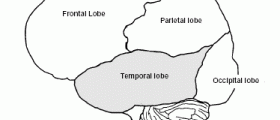
Benign rolandic epilepsy typically starts in childhood and is more reported in boys. There is no damage to patient's intelligence or disability of any kind. These seizures are called rolandic because they stem from abnormal electrical activity in the region around the lower portion of the Rolandic fissure.
Benign Rolandic Epilepsy - Clinical Characteristics
Benign rolandic epilepsy is associated with Somatosensory stimulation of the oral-buccal cavity, speech arrest, preservation of consciousness, excess of saliva production and tonic or even tonic-clonic activity of facial muscles. Sometimes the abnormal activity may transfer to the parts of the brain controlling the arms.
As far as characteristics of benign rolandic epilepsy affecting the motor sphere are concerned, the attacks remain localized on one side of the body even if the attack progresses into tonic, tonic-clonic seizures. The abnormal movement affects the face, arms or sometimes even legs.
Arrest in speech is noticed in the beginning of the attack and may remain during the entire episode of seizures. Fortunately, most patients remain conscious throughout the entire attack. At the end of the attack, the child may feel numbness, 'pins an needles' sensation, abnormal sensation in the tongue, gums and cheek on one side.
Nocturnal seizures are accompanied by clonic movement of the mouth and excess saliva production which is blamed for gurgling sounds coming from the throat. There is chance that nocturnal seizures progress into generalized seizures.
EEG -Electroencephalography
Benign rolandic epilepsy can be easily confirmed because of a distinctive patter reported during EEG. So after taking patient's medical history and performing a neurological exam doctors usually suggest EEG. Once EEG records the typical pattern associated with benign rolandic epilepsy, there is no need for further examinations and the condition is finally confirmed. Even though some doctors may recommend MRI of the head, this imaging study will not reveal any damage to the brain and is, therefore, no need to be performed.
Fortunately, in the majority of cases seizures of this type cease by the age of 15.














Your thoughts on this
Loading...