
Posttraumatic epilepsy is acquired condition associated with damage to certain parts of the brain. This type of epilepsy develops as a result of head trauma or is a side effect of certain surgeries preformed on the brain.
It is essential to differentiate posttraumatic epilepsy from posttraumatic seizures. Namely, posttraumatic seizures also occur as a consequence of brain injury. If they affect patients within 24 hours after the injury, they are classified as immediate posttraumatic seizures. Those that occur within a week are early posttraumatic seizures while seizures lasting more than a week after a brain injury are classified as later posttraumatic seizures. However, if these seizures eventually stop and never reoccur again they are never classified as posttraumatic epilepsy. Posttraumatic epilepsy is, therefore, a long term condition caused by brain injury.
Posttraumatic Epilepsy Pathophisiology
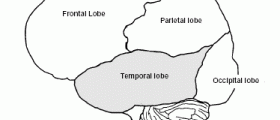
The very connection between trauma and the onset of such epilepsy has not actually been identified. It seems that lesions in the cortex play crucial role in triggering posttraumatic epilepsy.
There are some theories regarding iron deposits that accumulate in the brain after blood extravasation. Furthermore, excess of glutamate is considered another cause of damage due to excitotoxicity it induces. Tests performed on animals pointed to a disruption of the blood-brain barrier as a possible underlying cause of this type of epilepsy.
Posttraumatic Epilepsy Etiology
Statistical data show that people younger than 5 years of age and older individuals (over 65 years of age) are highly susceptible to this type of epilepsy. Furthermore, posttraumatic epilepsy is frequently reported in chronic alcoholism. This is explained by repeated falls and proneness to head and brain injuries which are typical for such addicts.
Posttraumatic epilepsy affects people with severe head trauma, those with penetrating head injuries as well as patients with intracranial hematoma. Furthermore, linear or depressed skull fracture, hemorrhagic contusion, coma lasting more than 24 hours and early onset of posttraumatic seizures are also likely to progress into posttraumatic epilepsy.Posttraumatic Epilepsy Prognosis
It is estimated that around 80% of all patients who have had some kind of head and brain injury will develop posttraumatic epilepsy within 2 years of the injury. Also the risk decreases gradually in time and becomes practically of insufficient importance 5 years after the injury.
Fortunately, around 50% of people who have developed posttraumatic epilepsy will enter a spontaneous remission.
Finally, if such epilepsy is confirmed, patients are prescribed appropriate treatment and must take their antiepileptic medications on a regular basis.














Your thoughts on this
Loading...