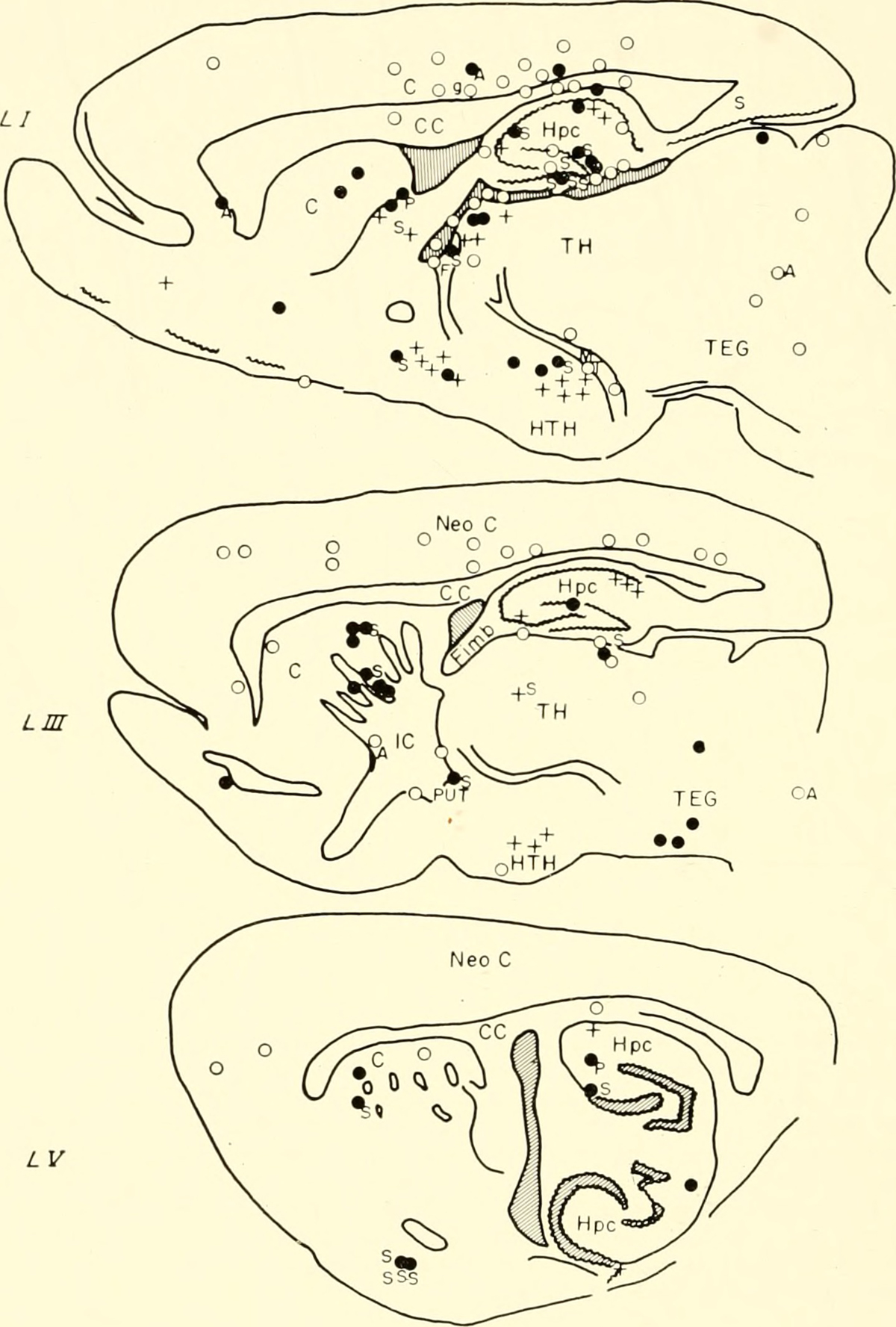
Epilepsia partialis continua is a medical disorder affecting the brain and its electrical activity. It is characterized by recurrent motor seizures that are solely localized to the hands and face. Seizures repeat every few seconds or minutes and may last for days or even longer.
Recurrent Motor Epileptic Seizures
The condition was first described in 1895 by Kojewnikoff, a Russian neurologist. He also named this type of epilepsy epilepsia partialis continua where each word practically describes the disorder. Epilepsy refers to seizures, partialis means that it remains localized and finally continua refers to the fact that attacks practically may last for a long period of time.
Seizures in individuals suffering from epilepsia partialis continua are focal motor clonic seizures without jacksonian march. They affect only certain parts of the body and abnormal motor activity may linger for hours, days, week and even longer. All patients remain conscious during the attack. However, most of them enter the postictal state. This is a changed state of consciousness that takes places after the attack. Namely, the person who has experienced seizures start to feel drowsy, confused, nauseated and may also have elevated blood pressure or headache. The postictal state may last from 5-30 minutes and it is the period when the brain actually recovers from the trauma triggered by seizures.
What Causes Epilepsia Partialis Continua?
The condition may have different causes which mostly depend on the age at which the first attack occurs. There are children suffering from this type of epilepsy and the disorder may occur in very old people. Many scientists believe that epilepsy as a health issue somehow begins at conception and that genetic traits play a significant role in the onset of the disease. Genes may also make people prone to epilepsy. Still, until more evidence is collected we can name certain factors and illnesses that are confirmed to trigger epilepsia partialis continua. In adults the disorder is associated with acute, large brain lesions that occur during stroke. In children, on the other hand, focal cortical inflammatory processes are the leading cause of the disease. Apart from the mentioned epilepsia partialis continua may also develop as a result of some chronic viral infections or is closely connected with underlying autoimmune processes.
Our genes are in charge of normal growth and development of each and every cell in the body, proper function of various hormones and enzymes and many different processes that are required for the entire body to remain healthy and well-functioning. So, if one is affected by genetically induced changes in chemicals and structures that make up the brain, he/she is at risk of certain disorder. One of these may be epilepsia partialis continua.
Furthermore, infection of the brain is considered a contributing factor in the onset of the disease. Namely, both encephalitis (inflammation of the brain) and meningitis (inflammation of the meninges) may easily interfere with the flow of electrical signals and trigger seizures during the active disease. Since in the majority of cases seizures last only during the infection this is not a reason for one to worry. However, it is possible for attack to reoccur once the disease is gone. So this clearly drives to conclusion that infections and inflammation of brain tissues and its membranes may easily progress into epilepsy.
Finally, proper growth and development of the brain, especially its neurons is of vital importance for impeccable functioning of the organ. If, for example, such growth and development is somehow disrupted, certain groups of neurons may become easily excited and a source of abnormal electrical activity. Structural brain abnormalities are, therefore, not only blamed for a variety of cognitive problems, behavioral issues and memory problems but they are also closely connected with the onset of epilepsy.
Treatment for Epilepsia Partialis Continua
Treatment for epilepsia partialis continua is rather challenging. There are medications but it may be quite hard to stop seizures and prevent their recurrence. The goal of the treatment is predominantly focused on prevention of secondary generalization. It is also important to identify the underlying disease that might have triggered seizures. Once this condition is brought under control, seizures may not reoccur.
If a person is suffering from encephalitis or meningitis seizures may stop once these two inflammatory diseases are cured. Still, there is possibility for the attacks to repeat. Such patients require anticonvulsant medications.
Brain tumors as well as treatment regimes patients suffering from brain tumors undergo may be blamed for seizures that repeat even after the tumor is removed.
As far as medications are concerned, they may not be successful in altering the course of the disease. Still, phenytoin and Phenobarbital are efficient in the majority of patients. Furthermore, corticosteroids and immunosupression may be beneficial for certain number of patients, particularly those with specific serum antibodies. Additionally, there is one of relatively efficient but still experimental approache called transcranial magnetic stimulation.
Finally, patients in whom none of the aforementioned treatments cannot help undergo multiple subpial transsections while hemispherectomy is indicated in refractory cases of Rasmussen encephalitis.














Your thoughts on this
Loading...