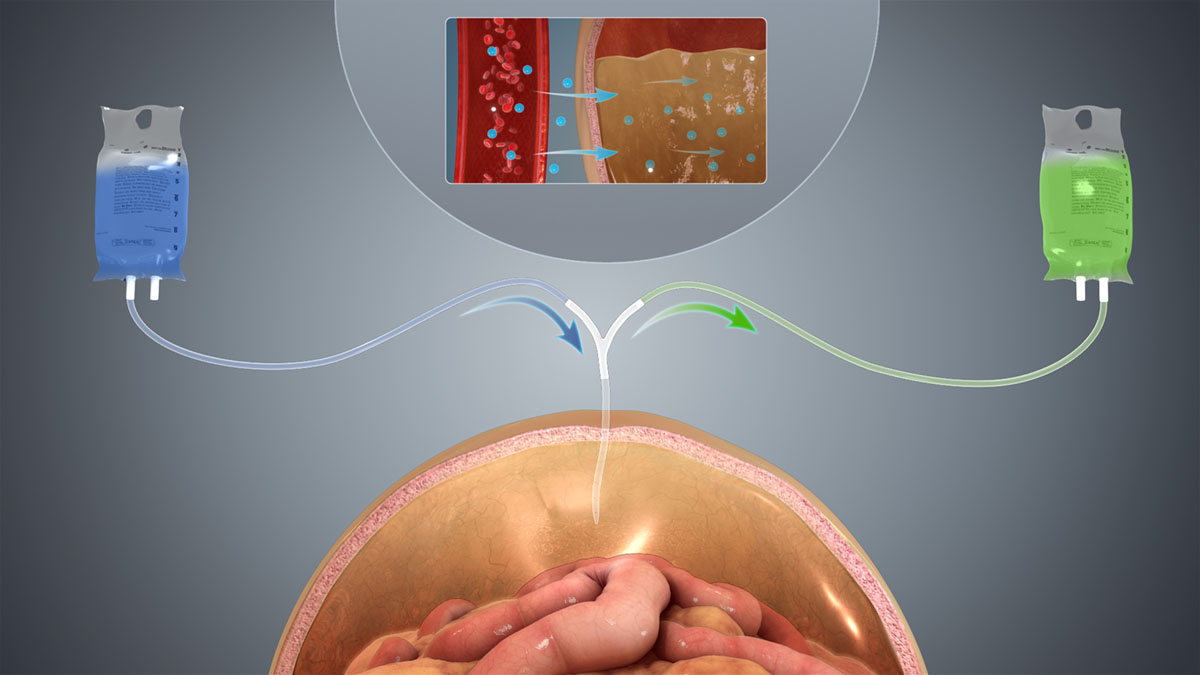
Peritoneal dialysis (PD) is an alternative procedure to chemodialysis for patients with severe chronic kidney disease. The patient's peritoneum is used as a film across which fluids and substances that are dissolved in it (electrolytes, urea, glucose, albumin and other small molecules) are rotated through the blood. Permanent tube in the abdomen is used to inject liquid that is used to purify the blood and also when the process is complete to pour liquid out. This method of dialysis has its advantages as well as its disadvantages. There is a possibility of performing dialysis without going to medical institutions but there is also a high risk of infection in the place where permanent tube is inserted in the abdomen. Catheter is surgically placed in the abdomen with one end attached to the skin surface. It is used to influence substantial amounts of liquid, about 2.5 liters, and before each infusion, area around the catheter must be disinfected. Dialysate remains in the abdomen and waste products diffuse across the peritoneum from the underlying blood vessels. Every four to six hours the liquid is poured out and in its place the fresh dose is poured in. This process is repeated six times within 24 hours. Sodium, chloride, lactate or bicarbonate and a glucose, used to provide hyperosmolarity, are the main ingredients of dialysate. The amount of liquid depends on frequency of dialysis and manufacturer of liquid.
Dialysate
There are several types of liquids and the way they affect the patient's blood. The exchange of fluid from the blood with glucose from the peritoneum is increased by the high concentration of glucose. Solution circulates from peritoneal cavity to the organs in order to enter the lymphatic system. It is not known why the amount of fluid that lymphatic vessels can absorb is different for every individual, and is referred to as high, low or intermediate level. If it is a high exchange level, substances need to be well soluble. In that way small molecules between the blood and dialysis fluids are quickly and easily exchanged and the results are improved. Low level carriers are better fluid filters (fluid transport through the membrane into the blood faster with somewhat better results with long-term, high-volume treatment), but in practice any type of conveyor is generally managed through appropriate use of either APD or CAPD.
Complications
Regular monitoring of quantities of liquids to be poured from the patient is needed. If the amount greater than 500 ml or even liter is lost during three processes of dialysis it can cause hypovolemic shock or hypotension, and in the opposite case, it may cause hypertension and edema. It is also important to monitor the color of fluid, which can be pink in the first couple of treatments and later should be clear or pale yellow. If the color is purple or there are traces of blood in the fluid, there is a possibility of internal bleeding. If the liquid is pale it can be a sign of infection.
If the fluid is too acidic, when the liquid is too cold or if it is injected too fast, it may cause discomfort or even pain.
Fluid can also increase pressure on the diaphragm causing difficulty with breathing. Constipation may interfere with the ability of fluid flow through the catheter.








Your thoughts on this
Loading...