Cellulitis is medical condition that shouldn’t be confused with cellulite, since this is medical condition. Acute infection of the skin, which has caused non-necrotizing inflammation, is considered to be the cause of this problem. Acute cellulitis affects the skin and subcutaneous tissues, but no muscles or fascia.
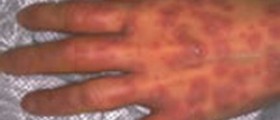
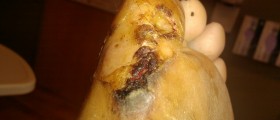
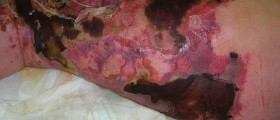
Patients usually complain about the pain, localized on some part of the body, tenderness, warmth, erythema and swelling on affected areas of the skin. This condition could also be presented with nodules, ulcerations on the skin along the present macular erythema.
Antibiotics for Cellulitis
About 90% of cellulitis patients respond well to antibiotic treatment, while all abscesses need to be surgically drained. Some patients with isolated cellulitis abscesses may not require antibiotics after drainage.
In general, patients with mild symptoms without some systemic diseases can be treated as outpatients. Extraction of the root canal and antibiotics are the therapy for facial cellulitis of odontogenic origin. Cool sterile dressings are recommended for removal of any purulent discharge, while elevation of the limbs affected with cellulitis is noticed to be beneficial for swelling. Slow response to antibiotic treatment may require long-term therapy with these drugs, in order to resolve present inflammation.
Patients treated with antibiotics may seem to gotten worse and experience increase of erythema, but this is just reaction to the drugs and situation usually gets better the following day. Person who develops some systemic symptoms, such as tachycardia or concomitant hypotension (low blood pressure) should be re-evaluated and considered for hospitalization.
Intravenous (IV) antibiotics are reserved for serious cases and patients who don’t respond to standard oral antibiotic treatment. Facial cellulitis, immune-supressed patients and those with elevated creatinine, creatinine-phosphokinase (CPK), C reactive protein (CRP) and low serum bicarbonate also indicate the need for IV antibiotics. Cardiac, hepatic or renal failure, as well as lymphedema patients should also receive IV antibiotics.
Recurrent cellulitis is treated with penicillin or erythromycin (if caused by Streptococcus sp.) and anti-fungal drugs if the cause of the problem is tinea pedis.
Surgical Procedures
Symptoms such as crepitus, necrotic skin, circumferential cellulitis, cellulitis that rapidly evolves or pain disproportional to physical problem should be consulted with the surgeon. Any clinical concern about necrotizing fasciitis and severe pains during passive movements should also be discussed with the surgeon, in order to decide whether the problem requires surgery.
Surgical drainage of abscesses or decompression of compartment syndrome may be needed surgical procedures in some cellulitis patients.Unusual cause of infection or no signs of improvement after standard treatments need to be consulted with specialist for infectious diseases.











Your thoughts on this
Loading...