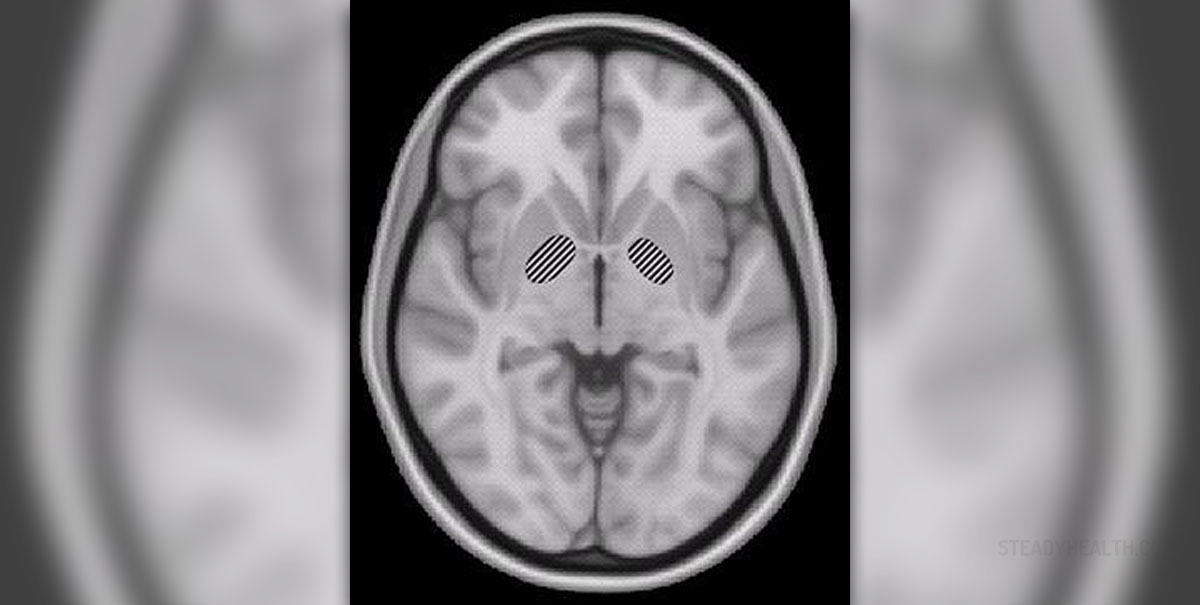
Parkinson’s disease is a member of neurological disorders, to be more precise it is a degenerative disorder resulting from the death of dopamine-generating cells. It is characterized by progressive neurological deficits. Initially, patients develop movement-related symptoms such as shaking, muscle rigidity and slowness of movement in general. There are also difficulty walking and gait. Further progression of the disease is closely connected with cognitive, behavioral changes as well as dementia, which is a characteristic of advanced stages of the disease.
Pallidotomy for Parkinson’s Disease
Pallidotomy is an invasive surgical procedure where the surgeon heats the globus pallidus with the assistance of a tiny electrical probe. The heating is restricted to 80°C and never exceeds one minute. The goal of the procedure is the destruction of a small area in the brain which is considered an underlying cause of dyskinesis, a common problem affecting individuals suffering from Parkinson’s disease.
The surgeons are precise enough to destroy the globus pallidus (one of the basal ganglia) and leave the surrounding tissues intact. The procedure is highly efficient when it comes to eliminating both tremor and rigidity associated with Parkinson’s disease.
Initially, patients with Parkinson’s disease receive medicamentous treatment. The drugs might be efficient in the beginning but they eventually stop working optimally and patients become more and more affected by neurological deficits and abnormalities. This is when pallidotomy might be indicated. As a matter of fact, pallidotomy is recommended if there are severe motor fluctuations (e.g. dykinesis or on-off responses) which generally develop as side effects of prolonged treatment with levodopa.
Furthermore, the surgery is an option if one deals with disabling tremor, severe muscle rigidity or bradykinesia (slow movement), all of which cannot be managed with suitable drugs any more.
And finally, pallidotomy is a good substitute for levodopa in patients who have not responded well to the drug. Some scientists say that even with the surgery these patients have low response rate.
The highly appreciated effect of the treatment is a significant reduction in dyskinesia precipitated by prolonged intake of levodopa. Patients may show rapid improvement soon after they have been operated. The dose of the drug will reduce and as a result many side effects will diminish or be completely eliminated.
Unfortunately, medical experts cannot say for sure for how long the effects of the surgery will last. Sometimes in spite of great initial response the positive effects of the procedure soon fade leaving patients with the same problems they had prior to the surgery.
Pallidotomy Procedure Safety
Prior to the procedure neurosurgeons use MRI scans of the brain in order to precisely located the area of interest. Patients remain awake throughout the surgery and only local anesthetics are used for numbing the scalp and the part of the skull which is going to be drilled for the purpose of further insertion of an electrical probe. Once the surgeons are sure they have entered the globus pallidus they use the probe and destroy the tissue. After this is done, the wound is closed.
Destruction of the globus pallidus on one side of the brain will improve dyskinesia affecting the other side of the body.
Patients remain hospitalized for a couple of days while the entire recovery lasts o longer than 6 weeks.
Most complications that used to be quite common in the past are today easily prevented. Even if some problems do occur, with adequate treatment these are successfully brought under control. MRI is of major help for identifying the precise location of the globus pallidus which was not possible many years ago and at that time damage was not solely restricted to the globus pallidus but sometimes additionally affected nearby tissue.
One of potential and rather serious complications of pallidotomy is brain hemorrhage (a stroke). Certain percentage of treated patients might fully recover from stroke and eventually benefit from pallidotomy.
Besides, there is a risk of cognitive impairment. This complication is practically irreversible. Infections and seizures may occur as well. If any of the aforementioned occurs, one will remain hospitalized for additional period of time and will require a suitable rehabilitation.
In spite of all the advantages of the procedure, pallidotomy is not commonly performed. Most medical experts recommend deep brain stimulation instead. This procedure is not associated with any damage to the brain and definitely carries less risk compared to pallidotomy.
All in all, pallidotomy is an invasive procedure but shows great results when it comes to patients suffering from Parkinson’s disease. It is not the first treatment option these patients are recommended. However, once their basic therapy starts to trigger many uncontrollable side effects and when the response to administered medications becomes insufficient or even absent, the procedure might deal with certain health issues these patients encounter. Pallidotomy is efficient against muscle rigidity and dyskinesia in general. Although there are risks associated with the surgery, these are reduced to minimum with improved pre and post-operative evaluation and care.





-When-You-Have-Parkinson's-Disease_f_280x120.jpg)










Your thoughts on this
Loading...